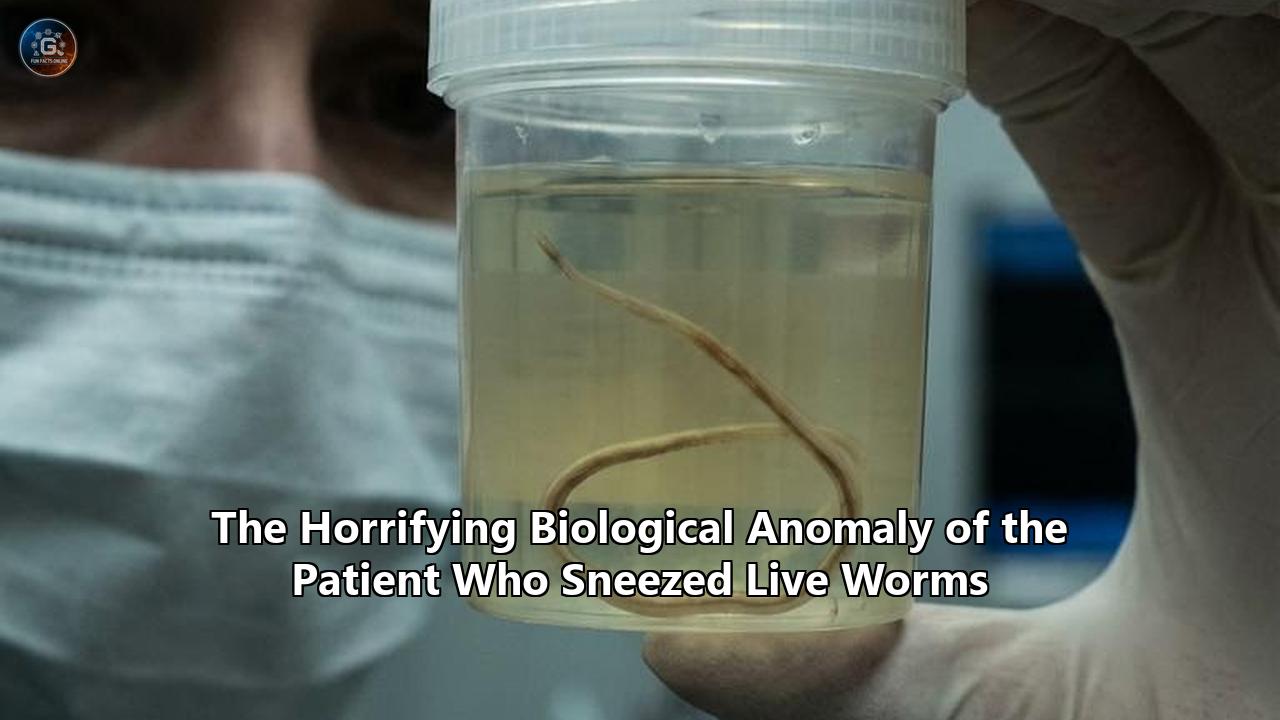
Medical professionals in Greece have just documented an unprecedented case of human parasitology that defies established scientific understanding of zoonotic infections. A 58-year-old woman working on a rural Greek island became the unwitting host to a colony of sheep bot flies (Oestrus ovis), culminating in a surgical extraction of 10 mature larvae and one fully formed pupa from deep within her facial cavities.
The case, detailed in medical reports this week, is making international headlines not just for its visceral shock value, but because entomologists and infectious disease experts previously considered this level of parasitic maturation inside a human sinus cavity to be "biologically implausible". Humans are accidental, dead-end hosts for Oestrus ovis. The human immune system, combined with the hostile architecture of our nasal passages, typically kills these larvae before they can grow.
Yet, due to a perfect storm of anatomical abnormalities and environmental exposure, this patient’s sinus cavity acted as an incubator, allowing the parasites to feed, grow, and reach a stage of development never before recorded in a human nasal cavity.
To understand how a routine day outdoors escalated into a medical horror story, we must trace the precise timeline of this infestation, the biological mechanics of the parasite, and the eventual clinical intervention that saved the patient from severe tissue destruction.
Phase I: The Strike (September)
The timeline of this medical anomaly begins in September, against the backdrop of a rural Greek island. The 58-year-old patient was working outdoors near a field heavily populated with grazing sheep. She reported noticing a large swarm of flies persistently buzzing around her face.
What she experienced was not a random nuisance, but the highly evolved predatory behavior of the adult female Oestrus ovis.
Unlike mosquitoes or ticks that land and bite to transmit parasites, the sheep bot fly operates like a biological stealth bomber. The adult female fly does not lay eggs in the environment; instead, the eggs hatch internally. The female fly carries live, highly mobile first-instar larvae (L1) inside her body. When she locates a suitable host—guided by olfactory cues and carbon dioxide emissions—she hovers near the face and rapidly squirts a liquid droplet containing roughly 20 to 25 live microscopic larvae directly into the nostrils or eyes.
This larviposition happens in a fraction of a second. The patient felt the flies swarming, but she did not feel the microscopic payload being deposited into her nasal vestibule. At approximately 1 millimeter in length, the L1 larvae immediately deployed their cephaloskeletons—specialized mouth hooks—to anchor themselves into her mucosal lining, preventing them from being expelled by a reflexive sneeze or the natural downward flow of mucus.
For the sheep bot fly, humans are an aberrant target. In a normal lifecycle, these larvae require the specific temperature, mucus composition, and anatomical layout of a sheep or goat's nasopharyngeal cavity to survive. When deposited in a human, the larvae usually perish rapidly. But in this instance, the parasites survived the initial breach.
Phase II: The Breach of the Maxillary Vault (Late September)
Within hours of the strike, the L1 larvae began migrating deeper into the patient's respiratory tract. Their target was the paranasal sinuses.
The human maxillary sinus is a pyramidal-shaped cavity located within the body of the maxilla (the upper jawbone), beneath the eyes and alongside the nasal cavity. Its primary defense mechanism is mucociliary clearance. The sinus is lined with pseudostratified ciliated columnar epithelium, featuring goblet cells that produce a constant stream of mucus. Millions of microscopic hair-like structures called cilia beat in a synchronized, wave-like motion to push this mucus—and any trapped debris or pathogens—upward against gravity, out through a small opening called the ostium, and into the nasal cavity to be swallowed or expelled.
The larvae had to fight this current. Using their anterior hooks and rows of backward-facing spines, they crawled upward through the middle meatus and forced their way through the ostium, dropping into the dark, warm, and mucus-rich environment of the maxillary sinus.
It was here that the patient's unique anatomy sealed her fate. Medical imaging later revealed that she possessed a severely deviated nasal septum—the cartilage and bone dividing the nasal cavity was sharply off-center.
A severe septal deviation alters the aerodynamics of the nasal airway and can obstruct the ostiomeatal complex, the primary drainage pathway for the anterior sinuses. In this patient, the anatomical distortion essentially trapped the larvae inside the maxillary vault. The narrowed escape routes and altered airflow prevented the natural expulsion of the parasites, providing them with an isolated, secure microclimate protected from the body's more aggressive immune responses.
Phase III: Symptomatic Escalation (Early to Mid-October)
Approximately one week after the initial exposure, the clinical symptoms began to manifest. The patient developed localized, dull aching pain centered around her face, radiating across the maxillary sinus area.
At this stage, the infestation was mimicking a standard bacterial or viral sinusitis. If she had visited a general practitioner at this point, the standard diagnostic protocol would likely have resulted in a prescription for antibiotics or corticosteroids, neither of which would have eradicated a macro-parasitic infestation.
Inside her face, the larvae were molting. The L1 larvae fed on the mucosal secretions and cellular debris, growing rapidly. They shed their outer cuticles and transitioned into the second larval stage (L2), growing from 1 millimeter to between 3 and 12 millimeters. The physical presence of these growing organisms triggered an inflammatory cascade. Mast cells and eosinophils flooded the sinus tissue, causing the mucosal lining to swell dramatically.
By the second and third week, the localized facial pain evolved into a severe, persistent cough. This was a secondary reflex symptom. The swelling of the sinus tissues, combined with the excessive production of mucus generated by the body in a desperate attempt to flush out the invaders, led to heavy post-nasal drip. The fluid irritated her pharynx and lower airway, triggering violent coughing spasms.
The L2 larvae continued to gorge, molting once more into the third and final larval stage (L3). At this point, the parasites were immense compared to their entry size. Entomological analysis would later measure the extracted pale yellow L3 larva at 0.6 inches (15 millimeters) in length, and a more mature light brown L3 larva at a staggering 0.8 inches (20 millimeters).
The physical movement of ten larvae, each nearly an inch long, crawling within the confined space of the maxillary sinus, caused severe mechanical irritation. They were rapidly depleting the available resources inside the sinus and preparing for their next biological imperative: exiting the host.
Phase IV: The Expulsion (October 15)
The turning point occurred on October 15. The L3 larvae, having reached maximum size, began seeking an exit. In their natural sheep hosts, this is the stage where the larvae migrate back through the ostium into the nasal passage, waiting for the animal to forcefully sneeze them out onto the soil.
The patient's severely deviated septum made this migration difficult, but the extreme irritation in her nasal cavity finally triggered a massive reflex.
During a violent spasm, the patient experienced the horrifying reality of sneezing live worms. A wriggling, one-inch-long larva was forcefully ejected from her nostril. The psychological shock of expelling a visibly active, segmented parasite from the center of her face prompted her to immediately seek emergency medical attention.
Sneezing live worms is an incredibly rare chief complaint in emergency medicine, particularly in developed regions. While physicians are trained to recognize various forms of bacterial, viral, and fungal sinusitis, finding a macroscopic arthropod emerging from a patient’s respiratory tract immediately shifts the diagnostic protocol from routine otolaryngology into the realm of tropical medicine and parasitology.
Phase V: Surgical Intervention and the Pupation Anomaly (Late October)
The patient was urgently referred to an Ear, Nose, and Throat (ENT) specialist. Given the gross evidence of the expelled L3 larva, an endoscopic examination of the nasal cavity was initiated.
Using a rigid nasal endoscope, the surgeon navigated past the deviated septum and examined the middle meatus and the maxillary ostium. The visual confirmation was stark: the sinus cavity was infested.
Because of the physical size of the larvae and the structural impediments caused by the deviated septum, conservative chemical treatments—such as topical ivermectin irrigation, which is sometimes used to paralyze and kill nasal bots—were deemed insufficient or too risky. Dead, calcified larvae left inside the sinus could trigger severe secondary bacterial infections, leading to sepsis or necrotic tissue damage. Surgical debridement was necessary.
During the surgical procedure, the ENT specialist successfully extracted 10 live, wriggling larvae from the mucosal folds of the maxillary sinuses.
However, it was the final object extracted from the sinus that elevated this case from a rare medical anomaly to a "biologically implausible" event. The surgeon removed a black, wrinkled, hardened casing.
Laboratory analysis confirmed that this casing was a puparium—the protective outer shell formed during the pupal stage of the insect. Inside the puparium were the remnants of a maturing pupa.
In the documented history of Oestrus ovis infestations in humans, this level of maturation is entirely without precedent. The life cycle of the sheep bot fly dictates that L3 larvae must drop onto the ground, burrow into the soil, and harden into a puparium. The pupal stage requires specific environmental temperatures and soil conditions, lasting anywhere from 3 to 9 weeks before the adult fly emerges.
For a larva to reach the L3 stage, initiate pupation, and form a hardened puparium entirely inside a living human host rewrites the known parameters of this parasite’s adaptability.
The Pathophysiology of the Impossible: Why Did They Survive?
Medical researchers analyzing this case had to answer a fundamental question: How did an obligate parasite of livestock manage to pupate inside a human skull?
The answer lies in a systemic failure of the human host's natural defenses, combined with an architectural anomaly.
Under normal circumstances, human cases of Oestrus ovis infestation (known as myiasis) are self-limiting. The flies most frequently deposit larvae in the conjunctival sac of the eye (external ophthalmomyiasis) or the outer nasal vestibule. In the vast majority of these cases, the larvae never progress past the L1 stage. The human basal body temperature, the specific pH of human mucosal secretions, and the aggressive response of our local immune system usually result in the larvae dying quickly, drying out, or being swept away by mucociliary clearance.
In this patient, several factors aligned to bypass these defenses:
- A Massive Initial Inoculum: The researchers hypothesize that the patient was inoculated with an exceptionally large larval burden during the initial fly strike. A higher volume of larvae increases the statistical probability that a few will survive the initial immune response.
- The Deviated Septum as a Vault: The structural deviation in her nasal septum acted as a mechanical barrier. It disrupted the normal aerodynamic flow of air and mucus that would typically help flush foreign bodies out. Instead, the larvae were pushed into the maxillary sinus and trapped.
- Microclimate Adaptation: Once sealed inside the maxillary sinus, the larvae were shielded from external environmental fluctuations. The persistent inflammation generated heavy mucus production, providing an endless food supply. The deviated septum prevented the larvae from escaping when they reached the L3 stage, forcing them to adapt.
- Forced Pupation: Unable to exit the host to find soil, at least one of the larvae advanced to the pupal stage purely out of biological desperation. The sinus cavity, isolated and warm, inadvertently mimicked the dark, insulated environment of subterranean soil.
"From a purely anatomic perspective," the report authors concluded, the combination of the high larval burden and the septum deviation prevented the organisms from exiting, permitting them to progress to the L3 stage and, astonishingly, pupation.
The Global Threat Matrix: Nasal Myiasis
While the pupation aspect of this case is wholly unique, the broader condition—nasal myiasis—is a recognized and highly dangerous medical phenomenon.
Myiasis is broadly defined as the infestation of live vertebrate animals with dipterous (two-winged) fly larvae, which feed on the host's living or dead tissue, liquid body substances, or ingested food. While Oestrus ovis is an obligate parasite of livestock that occasionally strikes humans, other fly species are far more aggressive.
The New World screwworm fly (Cochliomyia hominivorax) and the Spotted flesh fly (Wohlfahrtia magnifica) are notorious for causing catastrophic human myiasis. Unlike the sheep bot fly, which generally feeds on superficial mucus and cellular debris, screwworm larvae actively burrow into healthy, living flesh.
When myiasis occurs in the nasal cavity, the anatomical risks are immense. The roof of the nasal cavity and the ethmoid sinuses are separated from the brain by the cribriform plate—a sponge-like bone that is perilously thin.
If nasal myiasis is left untreated, the relentless feeding and burrowing of the maggots can lead to severe complications, including:
- Extensive Tissue Destruction: The larvae secrete proteolytic enzymes that dissolve human tissue, leading to the necrosis of the nasal cartilage and the palate.
- Orbital Invasion: The parasites can migrate laterally through the thin lamina papyracea, invading the orbit of the eye, causing blindness and severe orbital cellulitis.
- Intracranial Penetration: The most fatal complication occurs when larvae burrow upward through the cribriform plate and enter the central nervous system. This can result in pneumocephalus (air in the cranial cavity), secondary bacterial meningitis, and death.
Historically, severe cases of nasal myiasis have been associated with vulnerable populations: the elderly, individuals with severe cognitive impairments, those with poor personal hygiene, or patients suffering from atrophic rhinitis (a condition that causes foul-smelling nasal crusts that actively attract flies).
However, as the Greek case demonstrates, even healthy adults with no cognitive impairments or underlying immunosuppression can fall victim if environmental exposure overlaps with subtle anatomical vulnerabilities like a deviated septum.
Looking Forward: A Changing Zoonotic Landscape
Following the complete surgical removal of the 10 larvae and the pupa, the 58-year-old patient was treated aggressively with nasal decongestants to reduce the mucosal swelling and restore normal sinus drainage. She required no further antimicrobial therapy and made a complete, uncomplicated recovery.
Yet, the resolution of her case leaves the medical and entomological communities with unsettling questions about the future.
The boundaries between human habitats and livestock zones are increasingly blurring. Furthermore, changing global temperature patterns are altering the active breeding seasons and geographical ranges of various fly species. Oestrus ovis, which typically limits its activity to the warmer months of spring and summer in temperate zones, may begin exhibiting extended periods of larviposition as winters become milder.
For the medical community, the primary takeaway is a necessary shift in diagnostic awareness. General practitioners and otolaryngologists, particularly those practicing in rural or agricultural regions, must maintain a higher index of suspicion for parasitic infections when presented with atypical sinus complaints. When a patient presents with severe, unilateral facial pain, a persistent cough, and a history of outdoor exposure, the differential diagnosis must extend beyond standard bacterial sinusitis.
The horrifying image of a patient sneezing live worms is a visceral reminder of our vulnerability. The human body is a complex fortress, guarded by an intricate immune system and physical barriers. But as this Greek medical anomaly proves, even the strongest biological fortresses have structural weak points. A simple deviated septum was all it took to turn a temporary nuisance into a dark, warm sanctuary, allowing a livestock parasite to rewrite its own biological rulebook inside the human skull.
Reference:
- https://www.livescience.com/health/viruses-infections-disease/diagnostic-dilemma-womans-biologically-implausible-infection-led-her-to-sneeze-worms-out-of-her-nose
- https://www.indiatoday.in/health/story/woman-sneezes-out-worms-in-rare-infection-doctors-call-biologically-implausible-2895017-2026-04-12
- https://www.hindustantimes.com/trending/woman-sneezes-1-inch-worms-after-rare-biologically-implausible-nasal-infection-101775708228815.html
- https://www.freepressjournal.in/viral/greek-woman-sneezes-out-large-worms-from-nose-in-rare-biologically-implausible-case
- https://en.wikipedia.org/wiki/Oestrus_ovis
- https://wcvm.usask.ca/learnaboutparasites/parasites/oestrus-ovis.php
- https://www.scops.org.uk/external-parasites/nasal-bots/
- https://ruminants.ceva.pro/oestrus-ovis
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6951102/
- https://en.wikipedia.org/wiki/Maxillary_sinus
- https://www.mdpi.com/1648-9144/58/5/672
- https://www.youtube.com/watch?v=kr6vRSBhc6Y
- https://www.researchgate.net/publication/13671273_Pathophysiology_of_Oestrus_ovis_infection_in_sheep_and_goats_A_review
- https://pmc.ncbi.nlm.nih.gov/articles/PMC3027854/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC6078220/